Ambriel vs Assured
Side-by-side comparison to help you choose the right product.
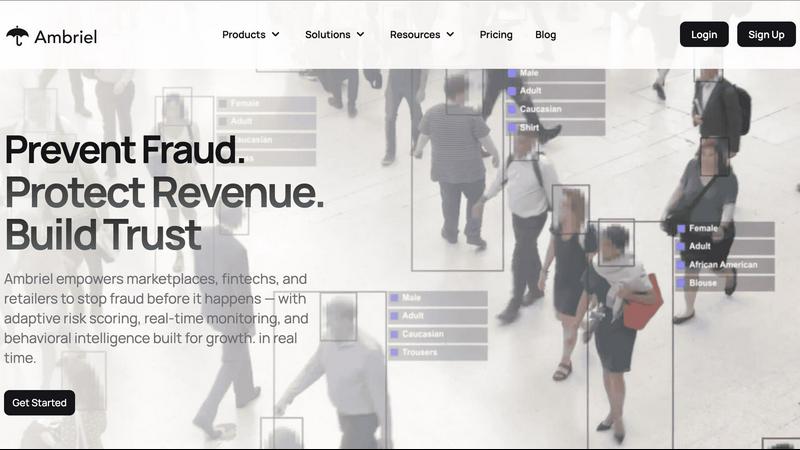
Ambriel provides real-time fraud detection and prevention to safeguard revenue and maintain customer trust across.
Last updated: March 1, 2026
Assured
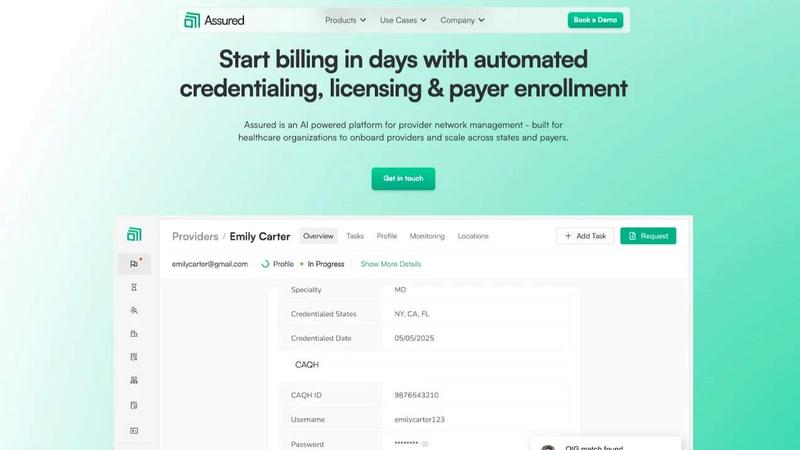
Assured is an AI platform that automates healthcare provider credentialing and enrollment to accelerate revenue cycles.
Last updated: April 13, 2026
Visual Comparison
Ambriel
Assured
Feature Comparison
Ambriel
Advanced Fraud Detection
Ambriel employs AI-driven risk scoring and leverages data from over 200 sources to identify suspicious activities in real-time. This robust feature helps protect revenue by addressing potential fraud risks before they escalate.
Sanctions & PEP Screening
The platform automates the screening process against over 100 global sanctions, PEP, and crime lists. This feature eliminates the need for manual checks, ensuring compliance while streamlining operational efficiency.
Continuous Monitoring
Ambriel provides 24/7 transaction and account monitoring, allowing organizations to track unusual patterns and behaviors. The system generates alerts for anomalies, enabling swift responses to potential fraud incidents before significant damage occurs.
Seamless Onboarding
With customizable onboarding flows that include automated checks, Ambriel ensures that only trusted customers and sellers gain access to the platform. This feature significantly reduces the risk of fraudulent accounts entering the system.
About Assured
AI-Powered Primary Source Verification
Assured's AI engine automates the verification of provider credentials by connecting to and cross-referencing data from over 2,000 primary sources simultaneously. This eliminates the need for manual, sequential data chasing across disparate websites and databases. The system instantly validates licenses, education, work history, sanctions, and malpractice history, ensuring the highest accuracy and dramatically reducing the verification timeline from weeks to hours, which is foundational to its 48-hour credentialing promise.
Automated Payer Enrollment & Submission
This feature streamlines the complex process of enrolling providers with insurance payers. Assured's platform auto-generates completed payer-specific applications using verified provider data and can submit them directly through integrated payer portals. It tracks each application in real-time, automates follow-ups, and manages payer-specific requirements, which collectively contribute to getting providers in-network approximately 30% faster and achieving a 95% first-pass approval rate.
Centralized Network Monitoring & Roster Management
Assured provides a single source of truth for all provider data. The platform continuously monitors verified information against primary sources for any changes, expirations, or new sanctions, alerting teams an average of 22 days earlier than manual methods. It supports centralized roster management, harmonizing data from various formats and systems to ensure accuracy for audits, contracting, and network adequacy reporting, eliminating last-minute surprises.
Integrated Licensing Management & Renewals
Managing state-specific licensing requirements and renewal deadlines is automated within Assured. The platform tracks expiration dates for all licenses across all 50 states, automatically initiates the renewal process, submits necessary applications, and handles state-specific paperwork. This removes the administrative chaos of multi-state expansion, ensuring providers remain compliant and able to practice without interruption due to licensure issues.
Use Cases
Ambriel
Onboarding & Registration Fraud
Ambriel effectively detects fake accounts, synthetic identities, and bot-generated signups during the onboarding process. This proactive measure prevents potential exploits from fraudulent actors before they can compromise the platform.
Payment & Transaction Fraud
The platform monitors real-time transactions to identify anomalies that may indicate fraudulent behavior. By preventing chargebacks and blocking unauthorized transfers, Ambriel safeguards businesses against financial losses.
Bonus & Promotion Abuse
Ambriel addresses issues related to multi-accounting and referral scams effectively. By stopping the exploitation of promotional incentives, this feature ensures that rewards are distributed fairly among genuine users.
Account Takeover Protection
Ambriel identifies unusual login behaviors, such as device changes and credential stuffing attempts. This capability protects customer accounts from unauthorized access, contributing to a secure user experience.
Assured
Scaling Digital Health Companies Across States
For digital health companies and telehealth providers expanding their services into new states, Assured is critical for managing the ensuing complexity of multi-state licensing and payer enrollment. The platform automates the research and submission process for each state's unique requirements, enabling rapid credentialing and network participation. This allows companies to scale their provider network efficiently and begin billing in days or weeks rather than months, directly supporting growth and patient access.
Streamlining Health System Provider Onboarding
Large health systems and hospitals can use Assured to overhaul their internal provider onboarding workflow. By automating primary source verification, credentialing, and initial payer enrollment through a centralized platform, Assured reduces administrative burden on internal staff, cuts onboarding time from over 60 days to a few days, and accelerates the point at which a new hire can generate revenue, thereby improving operational efficiency and reducing costs.
Ensuring Continuous Compliance for Payer Organizations
Health plans and payer organizations utilize Assured's network management capabilities to maintain accurate and compliant provider directories. The platform's real-time monitoring of sanctions, license expirations, and credential updates ensures network adequacy and compliance with state and federal regulations. This proactive approach mitigates audit risk and financial penalties while ensuring members have access to qualified, in-network providers.
Accelerating Market Entry for Provider Groups
Specialty provider groups, such as dermatology or behavioral health practices, use Assured to quickly credential new providers and get them enrolled with key payers when entering a new market or adding a new service line. The automation of manual tasks allows these groups to overcome administrative bottlenecks, reduce the time patients wait for appointments, and start generating revenue from new providers significantly faster than traditional methods allow.
Overview
About Ambriel
Ambriel is a state-of-the-art fraud intelligence and risk management platform tailored for digital businesses across various industries, including fintech, retail, marketplaces, and iGaming. Its core mission is to provide a secure and compliant environment that not only protects organizations but also safeguards their users from fraudulent activities. By utilizing advanced technologies such as behavioral analytics, device intelligence, and real-time risk scoring, Ambriel creates a comprehensive ecosystem designed to prevent fraud efficiently. The platform analyzes transactions, user behavior patterns, and network signals to identify hidden risks, enabling automatic threat mitigation. With Ambriel, businesses can proactively detect and prevent fraudulent scenarios such as multi-accounting, bonus abuse, and payment fraud, thereby preserving revenue and maintaining customer trust. This innovative solution empowers organizations to foster secure relationships with users while efficiently managing compliance with regulatory obligations.
About Assured
Assured is an AI-powered, NCQA-certified Credentials Verification Organization (CVO) and comprehensive provider network management platform engineered specifically for the healthcare industry. It is designed to automate the traditionally manual, error-prone, and time-consuming administrative processes that hinder operational scalability and revenue generation. The platform's core functionality addresses credentialing, licensing, payer enrollment, and ongoing network monitoring by leveraging artificial intelligence to verify credentials across more than 2,000 primary sources in parallel. This technological approach solves the critical problem of disconnected data systems and slow manual work, which typically delays provider onboarding by 45 to 60 days and results in significant revenue leakage. Assured's primary value proposition is delivering dramatic improvements in speed and accuracy: enabling provider credentialing in as little as 48 hours, achieving 95% first-pass approval rates for payer enrollments, and detecting sanctions 22 days earlier than manual methods. The platform serves a wide range of healthcare organizations, including provider groups, health systems, payers, and digital health companies, providing them with a single, centralized system to onboard providers faster, ensure continuous compliance, and accelerate time-to-revenue with complete data visibility and peace of mind.
Frequently Asked Questions
Ambriel FAQ
How does Ambriel help businesses comply with regulations?
Ambriel assists businesses in meeting compliance requirements through automated sanctions and PEP screening, continuous monitoring, and adherence to international standards like PCI DSS and GDPR.
What industries can benefit from using Ambriel?
Ambriel is versatile and can benefit a range of industries, including financial services, retail, e-commerce, marketplaces, iGaming, insurance, and cryptocurrency sectors, all needing robust fraud prevention solutions.
Is Ambriel easy to integrate with existing systems?
Yes, Ambriel offers integrations with various platforms, including Magento, WooCommerce, and Wix Commerce, making it easy for businesses to incorporate its fraud prevention features into their existing workflows.
Can I start using Ambriel for free?
Yes, Ambriel provides a free trial option, allowing businesses to explore its features and capabilities before committing to a paid plan, making it accessible for organizations to evaluate its effectiveness.
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Assured reduces onboarding time by automating the sequential, manual steps of traditional credentialing. Its AI performs parallel verifications across 2,000+ sources, cutting credentialing to 48 hours from 60+ days. By automating enrollment and licensing tasks, it reclaims over 60 hours of administrative work per week. Organizations save an estimated $4,200 to $5,800 per provider annually by reducing labor, accelerating revenue cycles, and minimizing errors that cause rework and delays.
What makes Assured more reliable than manual processes or other vendors?
Assured's reliability stems from its NCQA-CVO certification, which mandates rigorous standards for verification accuracy, and its use of AI for parallel, real-time data checks directly at primary sources. This eliminates human error and data lag inherent in manual spreadsheets and siloed systems. The platform's 95% first-pass payer approval rate and ability to detect sanctions 22 days earlier are quantifiable proofs of superior reliability and proactive compliance management.
Can Assured integrate with our existing systems like an ATS or EMR?
Yes, Assured is built with interoperability in mind. It offers plug-and-play APIs that allow for seamless integration with existing organizational systems, including Applicant Tracking Systems (ATS), Electronic Medical Records (EMR/EHR), and CRM platforms like Salesforce. This ensures provider data flows smoothly between systems, eliminates duplicate data entry, and creates a connected workflow from recruitment through to credentialing and practice management.
What kind of support can we expect during implementation and ongoing use?
Assured provides dedicated support with an industry-leading under 24-hour response time guarantee. Implementation includes expert guidance to configure the platform for your organization's specific payers, states, and workflows. Ongoing support is available to address questions, manage complex cases, and ensure your team can maximize the platform's value, contributing to a smooth operational experience and rapid issue resolution.
Alternatives
Ambriel Alternatives
Ambriel is a state-of-the-art fraud intelligence and risk management platform that helps digital businesses in sectors such as fintech, retail, marketplaces, and iGaming detect and prevent fraud in real-time. By employing advanced technologies like behavioral analytics and device intelligence, Ambriel safeguards revenue and builds customer trust through effective fraud prevention strategies. Users often seek alternatives to Ambriel for various reasons, including pricing considerations, specific feature sets, or compatibility with their existing platforms. When evaluating alternatives, it's essential to assess aspects such as the robustness of fraud detection, compliance capabilities, ease of onboarding, and the level of continuous monitoring to ensure that the replacement solution meets the organization's unique needs.
Assured Alternatives
Assured is an AI-powered provider network management platform in the healthcare productivity and management category. It automates credentialing, payer enrollment, and compliance monitoring to help organizations scale efficiently and accelerate revenue. Users may explore alternatives for various reasons, such as budget constraints, specific feature requirements not covered by the platform, or a need for a solution that integrates with a different set of existing practice management or EHR systems. The search often stems from a desire to compare capabilities, pricing models, and implementation support. When evaluating alternatives, key considerations should include the depth of automation for credentialing and enrollment workflows, the platform's accuracy and speed metrics, compliance certifications like NCQA CVO status, and the robustness of real-time monitoring and reporting tools. The ideal solution should centralize data, reduce manual effort, and demonstrably shorten the time to revenue.
